 Keratoconus is degeneration of the structure of the cornea. The cornea is the clear tissue covering the front of the eye.
Keratoconus is degeneration of the structure of the cornea. The cornea is the clear tissue covering the front of the eye.
The shape of the cornea slowly changes from the normal round shape to a cone shape.
Causes, incidence, and risk factors
The cause is unknown, but the tendency to develop keratoconus is probably present from birth. Keratoconus is thought to involve a defect in collagen, the tissue that makes up most of the cornea.
The exact cause of keratoconus is not fully understood, but various factors are believed to contribute to its development. Here are some of the key factors:
- Genetics:
- Keratoconus often runs in families. If someone has a parent or sibling with keratoconus, they may be at higher risk of developing the condition.
- Oxidative Stress:
- The cornea cells produce byproducts like free radicals which are usually neutralized by antioxidants. However, if this balance is disrupted, oxidative stress can occur, which may lead to keratoconus.
- Eye Rubbing:
- Vigorous eye rubbing is thought to be a risk factor for keratoconus. It’s believed that the mechanical trauma from rubbing can thin the cornea and change its shape.
- Allergies:
- Individuals with allergies may rub their eyes frequently, which may contribute to the development of keratoconus.
- Hormonal Changes:
- Keratoconus often first appears in the teenage years or early twenties, suggesting that hormonal changes might play a role.
- Other Eye Conditions:
- Conditions like retinopathy of prematurity and other eye diseases might be associated with keratoconus.
- Contact Lens Wear:
- Poor fitting or hard contact lenses can also be a risk factor, especially if worn for extended periods.
- Environmental Factors:
- Some studies suggest that environmental factors might also play a role, although the exact relationship is not well established.
Also, there is an association between keratoconus and Down syndrome.
Symptoms
The earliest symptom is a subtle blurring of vision that cannot be corrected with glasses. (Vision can generally be corrected to 20/20 with rigid, gas-permeable contact lenses.)
Most people who develop keratoconus start out nearsighted. The nearsightedness tends to become worse over time.
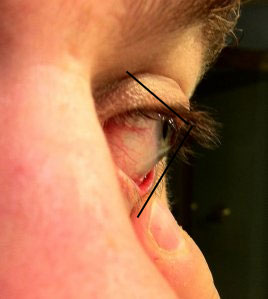 Signs and tests
Signs and tests
Keratoconus is often discovered during adolescence. It can usually be diagnosed with a slit-lamp examination of the cornea. The most accurate test is called corneal topography, which creates a map of the curve of the cornea.
When keratoconus is advanced, the cornea will be thinner at the point of the cone. This can be measured with a painless test called pachymetry.
Prevention and Treatment
Contact lenses are the main treatment for most patients with keratoconus. Severe cases may require corneal transplantation as a last resort.
- there are several treatment options available to halt or slow down its progression, manage symptoms, and improve vision quality:
- Corneal Cross-Linking (CXL):
- This is a common treatment for halting the progression of keratoconus. It strengthens the corneal tissue by creating new links between collagen fibers within the cornea.
- Contact Lenses:
- Specialized contact lenses, like rigid gas permeable lenses or hybrid lenses, can help in reshaping the cornea and improving vision.
- Intracorneal Rings or Intacs:
- These are small, plastic segments implanted within the cornea to flatten it and improve vision. They can also halt the progression of keratoconus to some extent.
- Topical Eye Drops:
- Sometimes, doctors may prescribe eye drops to control eye rubbing which can worsen keratoconus.
- Lifestyle Adjustments:
- Avoiding eye rubbing and wearing eye protection during sports or high-risk activities can help prevent further damage to the cornea.
- Corneal Cross-Linking (CXL):
Expectations (prognosis)
In most cases, vision can be corrected with rigid gas-permeable contact lenses.
If corneal transplantation is needed, results are usually good (read my corneal surgery diary.) The recovery period can be long, and patients often still need contact lenses.
Complications
There is a risk of rejection after corneal transplantation, but the risk is much lower than with other organ transplants.
Patients with even borderline keratoconus should not have laser vision correction. Corneal topography is done before laser vision correction to rule out people with this condition.
